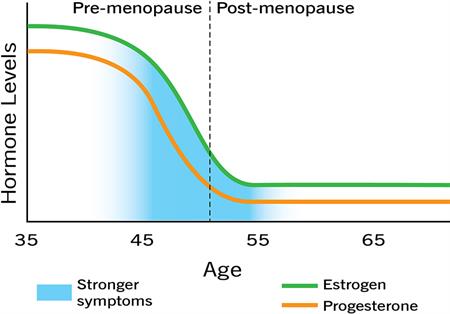
In my previous post, we learned about perimenopause (also known as pre-menopause) and that there are three stages of menopause:
- Perimenopause
- Menopause
- Postmenopause
Remember I mentioned how being “in menopause” seems like a misnomer since menopause isn’t a discrete event? Well, I also feel that way about classifying menopause in stages. It gives the impression that there are clear delineations between each phase and what happens within each stage. That’s not exactly the case.
- Menopause starts when you have your final period. But if the main symptom of perimenopause is irregular periods, when your last period starts, you have no way of knowing that it is actually your last.
- From a medical perspective, menopause is the point when a person* no longer has periods for at least 12 months.
- Postmenopause is the period after menopause.
By the time you can be clinically diagnosed as menopausal, you’re already postmenopausal!
Who came up with these confusing delineations?**
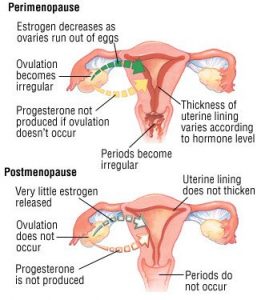
Perimenopause may start when you are in your 30s, 40s or 50s. For some, this phase lasts months and for others, a decade. You are still pre-menopausal unless you haven’t had a period for 12 consecutive months.
Signs that you are in perimenopause include: 1) irregular periods; 2) perimenopausal symptoms; and/or 3) elevated follicle-stimulating hormone (FSH) levels in your blood. You still can get pregnant during perimenopause, but not when you are postmenopausal. After 12 months without periods, your ovaries no longer are producing eggs.
Much like perimenopause, menopause and postmenopause impact people differently. The average age to experience natural menopause in the United States is 51. However, the age range varies with a 20-year spread. Menopausal symptoms generally abate in frequency and severity after your last period, but this also depends on the individual.
The average person still experiences menopausal symptoms for four years after their last period with a range of 1-10(!) years!
If you experience troublesome menopausal symptoms, you may wish to speak with your internist or GYN to evaluate whether you are a candidate for hormonal-replacement therapy (HRT). (And, by troublesome, this is troublesome for you. There is no objective standard here.) By restoring the hormones levels that change during menopause, HRT has been shown to successfully alleviate menopausal symptoms for many individuals. If your body responds well to HRT, consult with your doctor annually to weigh the benefits and risks of continuing the treatment. Most people stop HRT once their menopausal symptoms abate. It’s important to note that if you have a history of stroke, blood clots or cancer, you might not be a candidate for HRT.
Once your periods cease and you are postmenopausal, you are at a higher risk of:
By this point in the post, if you haven’t uttered, “Ughhhhhh!” or some variant of that, feel free to do so now. Then I recommend reminding yourself that menopause is a part of life, and you will adjust to the changes that ensue as you have to previous life and health changes. And, whatever phase you are at with menopause and your acceptance of the process, know I’m only a message or comment away!
In my next posts, I’ll write more about postmenopausal health risks, the stigma surrounding menopause, my menopause journey, and how to find community and support during menopause. Until then, be well xoxo
* Since 2008, the majority of my posts were written as though everyone with a vagina identified as female. I know better now and am trying to approach this post correctly using gender-inclusive language.
** The American Society for Reproductive Medicine classified the stages of menopause. “Menopause” comes from the Greek words for mēn (month) and paûsis (pause), and Aristotle is credited with one of the early references to the term.

Disclaimer: Although I wear many hats, I’m not a doctor nor do I play one on TV. This post is not a substitute for medical advice. Hyperlinks are plentiful in this post to help steer you toward additional information from reliable medical sites.